Costing community health and social services
In the Republic of Ireland, Health Service Executives (HSE)s combine many of the services that in the UK are split between Health and Social Services. The HSE Southern Area is responsible for the two counties of Cork and Kerry, an area roughly 150 miles by 100 miles, and spends €850 million per annum. It needed to know if it was spending the money well, and what drove expenditure, by being able to answer such questions as “How will changes in the population put demands on our health services?”, Can we influence future demands on social services through health education and preventive care?”, Are there better, more cost effective ways of providing our full range of services?”.
The Activity Based Costing (ABC) approach was chosen as an ABC analysis was able to throw more light on why costs exist and how they vary. Instead of starting with how much was spent last year compared to budget, ABC concentrates on what the money is being spent on, and why it is spent. For example, how much does a Home Help really cost, and how many people will need such help next year? Will an ageing population influence the number of people needing community facilities? What is the trend in drug abuse, and therefore how much do we need to budget to deal with it? Can we influence demand for services through health promotion?
ABC analysed the whole cost of providing treatments and services – not just the direct clinical and service costs, but other support costs such as accommodation, equipment, management, administration and information technology. Armed with the ABC information, future submissions to the Department of Health and Children are based on proven costs of activities and their cost drivers, which ensure that adequate and realistic budgets are put in place.
- Adoption Services
- Aftercare Services
- Assisted Living Services
- Aural Services
- Cardiovascular Strategy
- Child Abuse Unit
- Child Care
- Children’s Residential Homes
- Chiropody Services
- Community Hospitals
- Day Centres
- Dental Services
- Dietetic Services
- Environmental Health Services
- Family Support Services
- Family Therapy Services
- Food Microbiology Laboratory
- Fostering Resource Unit
- Health Promotion Dept
- Home Helps
- Homeless Adults
- Immunisations
- Infectious Disease
- Medical Card Assessment
- Mercy Childcare Transfer
- Nursing Homes
- Occupational Therapy Services
- Ophthalmic Services
- Palliative Care Services
- Pharmacy Services
- Physical & Sensory Disabilities
- Physiotherapy Services
- Pre-School Services
- Psychology Services
- Public Analyst Laboratory
- Public Health Nursing
- Refugee Services
- Residential Homes Inspect
- STD/Aids Clinics
- Screening - Asylum Seekers
- Social & Health Education
- Social Work Services
- Special Housing Aid
- Speech & Language Therapy
- Substance & Alcohol Abuse Services
- Surveillance
- Travellers' Services
- Voluntary Bodies
- Young People Special Care Units
The HSE Southern Area ABC Model
In total the HSE has 18,000 staff, based in 250 separate buildings and has a spend of €850 million. The Acute hospitals were excluded from the analysis in the initial phase.
The scope of the ABC model was Community Hospitals (€40 million) and Services (€260 million) and those Central Services’ costs that were focused on supporting the community (€68 million). Depreciation costs from the Asset Register added another €17 million into the model. Overall, the ABC model included 470 Cost Centres and a total of 10,288 Ledger Lines!
The costs were assigned from the ledger (the resources) to activities and then onwards to nearly 50 different services.
Looking at the detail
| Service | Activities | Activity cost €s | Cost driver | Volume | Unit cost |
|---|---|---|---|---|---|
| Adoption Services | Inter country adoption assessments | 399,581 | # IC Assessments | 144 | 2,775 |
| Post placement visits | 33,992 | # Visits | 47 | 723 | |
| Search and reunion | 67,984 | # Searches | 45 | 1,511 | |
| Assessment for domestic adoption | 55,000 | # Assessments | 5 | 11,000 | |
| Placement for domestic adoption | 94,493 | # Mothers seen | 37 | 2,554 | |
| Total service cost | 651,050 | ||||
Taking the first service, Adoption Services, the ABC model determined the costs of the constituent activities. Knowing the cost drivers for each activity and the cost driver volume allowed the unit costs to be determined. These are shown in the table shown above.
Tunneling into the data threw up useful comparisons that raised many questions. For example, why does home help cost a third more in one area than another? (see table below)
| Care of older person | # Patients | Total cost | Unit cost |
|---|---|---|---|
| Home helps (Kerry) | 2,097 | 5,516,496 | 2,631 |
| Home helps (North Lee) | 1,761 | 3,458,230 | 1,964 |
The ABC model determined the costs of various treatments. The patients received the treatments so that the total cost of supplying health services to patients was determined. The patients also had differing attributes, the key one being age. Now costs could be shown by age group and per head of population within each age group.
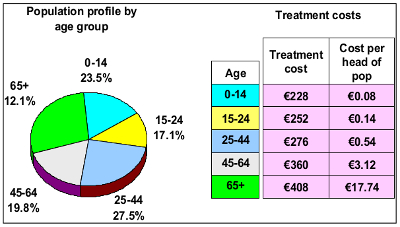
The costs and age profiles are shown in the diagram right.
From other sources, changes in the demographic profiles over time and by region could now be linked to health costs. The overall demographic profile could now be used to give an accurate forecast of the demands on the health system.
Other major benefits were the enhancement of budgeting and control, the ability to analyse and understand costs and where appropriate to seek reductions. It also provided the capacity to develop performance management modelling thereby generating meaningful management information, which allowed better decisions to be made on service delivery at local level.
The costing of Community Services is notoriously difficult; as activity and cost data is not as sophisticated or as readily available as in the acute sector. But with the ABC project the Health Service Executive met a number of key objectives:
- It achieved transparency of costs
- It better understood value for money
- It linked demographic changes to resources
- It linked Government policy to resources
- It could better plan services provision

